Gestational surrogacy, also known as the host method, happens when the eggs of another woman have been fertilized and the resulting embryo put into the uterus of the surrogate. In general, you and your partner will experience an assisted reproductive technology (ART) procedure such as in vitro fertilization (IVF) to generate an embryo that is biologically yours. If this is not possible owing to the nature of your fertility problem, you could also make use of donated eggs, sperm, or embryos. Your embryo will subsequently be put in the uterus of a gestational carrier, who will take the baby to term. When the child is born, the carrier will turn the baby over to you and sign her parental rights.
Usually, gestational carrier arrangements are set up either as independent adoptions, in states where they are legal, or more commonly by contracts arranged through agencies. Some physicians focus in working with gestational carriers and could help you in making an arrangement. Most likely, you will be deeply involved in the pregnancy.
Advantages to Gestational Surrogacy
- The emotional link between the surrogate and the child is not as strong as it could be if the child was genetically her own.
- With this method, an intended mother who was able to offer her own eggs would have a biological link to any resultant children.
- There is also the aptitude to make use of an older surrogate as the eggs provided for in vitro fertility will be from a much younger source.
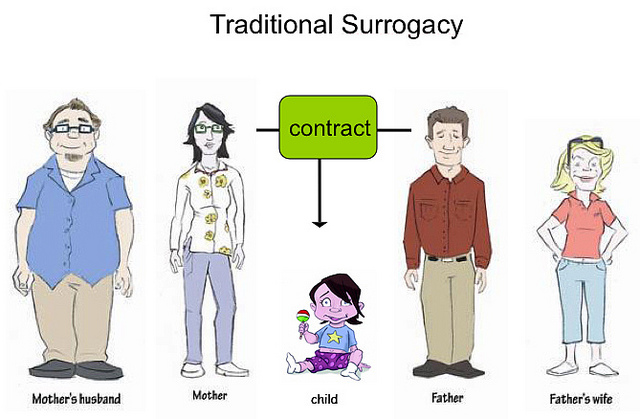
Traditional Surrogacy
Also known as Partial Surrogacy, Traditional surrogacy employs your own sperm, or that of your partner, to inseminate the surrogate using the surrogate’s own egg. In this method, the surrogate is also the genetic parent of any children resulting from that pregnancy. In traditional surrogacy, the surrogate’s egg is fertilized using artificial insemination, and this for a long time was the only available option for couples looking to employ surrogacy, and is considerably less expensive than IVF. There is a high success rate when using a surrogate with an established fertility, and the rebound time after a failed attempt is a matter of weeks.There are a few ways of really executing the inseminations: Doctors become inclined to execute intrauterine inseminations (IUIs) or intra-cervical inseminations (ICIs) relying on the quality of sperm, whether the sperm is fresh or frozen. In an ICI, a small catheter is used to put the semen inside the surrogate’s cervix. IUIs are executed only with washed sperm: semen that has been sent through a centrifuge and spun until the seminal fluid is taken away and only the strongest sperm cells stay. A catheter is threaded through the cervix into the uterus, and the sperm are put in through it into the uterus directly. In general, traditional surrogates do not have to be on any special medications. They keep an eye on their own menstrual cycle and time the inseminations around when they naturally ovulate. In some cases, intended parents and their surrogate will decide to employ mild fertility drugs, such as Clomid, to fine-tune the timing of ovulation or enlarge the chances of twins.
Through charting her basal body temperature, watching her cervical mucous, and employing ovulation predictors or fertility monitors, and/or through ultrasound monitoring by a clinic, the surrogate could identify when she is most likely to ovulate and arrange inseminations to agree with this.
 Gestational Surrogacy Gestational Surrogacy India: A Hub of Surrogate Mother Delhi
Gestational Surrogacy Gestational Surrogacy India: A Hub of Surrogate Mother Delhi